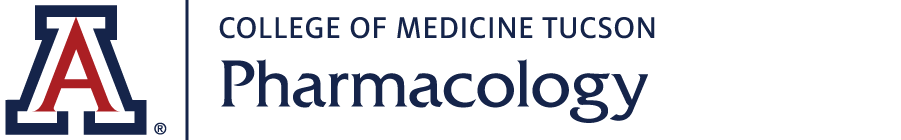Pathways discovered where Blood Brain Barrier (BBB) tight junction and specific transporter proteins can be targeted to improve CNS drug delivery in neurological disease states. We continue to help define the concept that the BBB can be targeted through signaling pathways, specific transporters, and/or drug:drug interactions. These identified pathways point to opportunities to enhance drug delivery in disease states associated with hypoxia, stroke and acute pain.
The focus of my research is the blood brain barrier /Neurovascular Unit (BBB/NVU) in health and disease and specifically the effects of stroke and acute pain on the BBB/NVU. The BBB plays a vital role in maintaining brain homeostasis. Composition of the brain interstitial fluid is controlled within a precise range, independent of fluctuations within the blood, allowing optimal neuronal function to occur throughout life. The BBB is situated at the cerebral endothelial cell tight junctions of the cerebral microvessels.
Figure.1. Schematic showing the BBB/Neurovascular unit. Note the association of NVU astrocytes to endothelial cells.
The cerebral endothelial cells form a continuous membrane with no fenestrations, unlike peripheral vessels. The endothelial cells of the BBB are connected via a network of protein tight junctions that create a rate-limiting, high transendothelial resistance (TEER) barrier to paracellular diffusion of solutes. Structurally, BBB tight junctions form a continuous network of parallel, interconnected, intramembrane protein strands, which are composed of an intricate combination of transmembrane and cytoplasmic proteins linked with the actin-based cytoskeleton, allowing the tight junction to form a cell:cell seal while remaining capable of rapid modulation and regulation by specific signaling molecules.
Figure 2. Schematic of the tight junctions of the BBB. Tight junctions consist of three main groups of proteins. They are transmembrane proteins (Claudins, occludin and junctional adhesion molecules), accessory proteins (ZO-1,2,3 to 20) and cytoskeletal structural proteins such as actin. All three groups interact to maintain the tight junctions with high trans endothelial resistance (for a more detailed review see Hawkins and Davis, 2005, or Ronaldson and Davis, 2013). These proteins can be modulated via several mechanisms. In neuroinflammatory CNS disorders (Alzheimers, Parkinsons and multiple sclerosis), alterations in these proteins contribute to disease progression.